What is the Diabetes Treatment?
Remember!
All the contents described here in the diabetes treatment page are current, accurate and reliable.
All the contents provided here are absolutely not medical advice or for medical diabetes treatment.
Those contents are for general knowledge, and educational purposes only.
This site's material and contents cannot replace a physician or a health care provider.
For further explanations, advice, and instructions you should address your private doctor or your diabetes educator.
The diabetes treatment is divided into three essential parts.
It must involve medicines, diet and exercise.
It is very important for you to understand it because your immediate goal is to reduce blood sugar levels.
A good diabetes treatment result will be controlling your blood sugar levels successfully.
Then, as a result, you will reduce symptoms and prevent complications.
The long-term goals are to prevent diabetes related complications and to prolong your life.
Oral Medicine
Diabetes pills can help controlling diabetes, but they cannot cure it.
 People with type 2 diabetes can use pills for their diabetes treatment, but not people with type 1 diabetes.
People with type 2 diabetes can use pills for their diabetes treatment, but not people with type 1 diabetes.
Those pills do not affect everyone the same way, and if they already have reduced your blood glucose levels they mostly haven't reduce it enough down to the normal range.
There is also the element of the sickness duration. People with diabetes for more than 10 years will be less affected then people who have developed diabetes recently or have
needed little or no insulin to keep their blood glucose levels near normal.
Those pills are sometimes taken only once a day, in the morning, although some people need for their treatment two or three doses.
More than one type of diabetes pill may be used if one is not adequate.
If oral pills cannot control blood sugar levels well enough, insulin injections alone or in combination with the pills may be needed for a better diabetes treatment.
There are several types of pills:
Sulfonylureas – pills that stimulates your Beta cells to produce more insulin into the blood. Pills such as: Amaryl, Diabinese, Glucotrol, Micronase.
They can often be taken once or twice a day.
Side effects: may cause hypoglycemia and weight gain, but it depends on how often the pills are taken, and interactions with other drugs.
Meglitinides – pills that also stimulates the Beta cells to produce more insulin into the blood, such as: Prandin and Starlix.
They can be taken before each of three meals.
Side effects: the same as of Sulfonylureas because of the stimulation of the insulin production.
Biguanides – pills that help insulin work better and increase the body's response to it. Pills such as Glucophage.
It can be taken two times a day.
Side effects: The Glucophage may cause diarrhea, but if the pill is taken with food the side effects will be minimal.
Thiazolidinediones – pills that make the body more sensitive to the insulin. Pills such as: Actos, Avandia.
Important note!
There were drugs in this group which were removed from the market:
There weren't any problems with the other drugs in this group but patients are still monitored closely for any problems as a precaution. Both drugs are effective at reducing A1C and generally have few side effects.
This drug was removed from the market because it caused serious liver problems in a small number of patients.
The U.S. Food and Drug Administration announced on Sept. 23, 2010 that it will significantly restrict the use of the diabetes drug Avandia to patients with Type 2 diabetes. For more details...
Alpha-glucosidase inhibitors – Acarbose and Meglitol are alpha-glucosidase inhibitors. These pills as a diabetes treatment can help the body to lower blood glucose levels by interfering with the absorption of sugar from the intestines after a meal. It can be taken with the first bite of a meal.
Side effects: These pills may cause abdominal pain, gas and diarrhea.
All those drugs work in different ways to reduce blood glucose levels.
You may combine some of them together in your diabetes treatment.
For example, a pill from the Sulfonylureas group and a pill from the Biguanides group can be taken together.
Many combinations can be used. The advantage of making such a combination is the improvement of the blood glucose control.
The disadvantage is that such a combination is more expensive and the risk for side effects is bigger.
Learn more about side effects of drugs here.
Insulin
In type 1 diabetes our body doesn't produce any insulin.
We have to complete this lack of insulin by taking insulin injections. If the pills in type 2 diabetes don't help either, in that case we have to take also the insulin injections.
The insulin cannot be taken by mouth because it is a protein and it would be broken down in the digestive system.
There are 3 types of insulin, and they divided by:
- Speed of onset.
- How much time until it gets to maximum activity.
- Duration of action.
Rapid-acting insulin - such as the regular insulin.
The regular insulin begins to work about 5 minutes after injection, reaches its maximum activity in 2 to 4 hours and works for 6 to 8 hours. The fastest ones are insulin lispro (Eli Lilly), insulin aspart (Novo Nordisk), or insulin glulisine (sanofi-aventis).
Intermediate-acting insulin – such as lente insulin, isophane insulin suspension, or insulin zinc suspension.
It starts to work in 1 to 3 hours, reaches its maximum activity in 6 to 10 hours, and works for 18 to 26 hours.
This type of insulin treatment may be used in the morning to provide coverage for the first part of the day or in the evening to provide coverage during the night.
Long-acting insulin – such as ultralente It starts to work 6 to 10 hours after injection and is usually effective for 20 to 24 hours. There are also two long-acting insulin analogues: glargine and detemir.
The insulin is injected under the skin into the fat layer. You can inject in the arm, thigh, buttocks, hip areas or abdominal wall.
The best recommended absorption site is the abdomen. Small syringes with very thin needles make the injections nearly painless.
Do not inject insulin near bony places or joints. Do not inject again in a point that is closer than 1 inch to the previous one.
You can repeat using the disposable insulin syringes with needles more than once, but it is very important to keep it clean.
Read here more about injecting insulin.
If you cannot tolerate needles you can use for your convenience an air pump device that blows the insulin under the skin.
There is also an insulin pen injector.
The insulin pen injector contains a cartridge that holds the insulin.
You screw a needle onto one end, dial the dose, and then inject.
The pen is a very convenient way for many people to carry insulin, especially for people who take several injections a day outside their home.
Read here more about insulin pens.
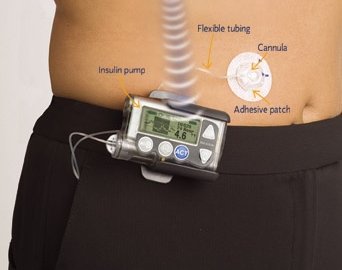
Another diabetes treatment device is the insulin pump.
The sequential injections are replaced here by the pump that delivers insulin continuously throughout the day using a catheter.
Using an insulin pump can improve your quality of life, because now you don't have to worry anymore about injections or swings in your blood glucose levels and you can continue with almost a normal lifestyle.
The insulin pump kit contains the pump itself (including controls, processing module, and batteries), a disposable reservoir for insulin (inside the pump), a disposable infusion set, including a cannula for subcutaneous insertion (under the skin) and a tubing system to interface the insulin reservoir to the cannula.
The pump delivers both a basal dose and a bolus dose.
The bolus dose is rapid-acting insulin that is pumped to cover food eaten or to correct a high blood glucose level.
The basal dose is slow-acting insulin that is pumped continuously at an adjustable basal rate to deliver insulin needed between meals and at night.
The insulin pump is a great responsibility.
First, you have to talk with your diabetes care team and learn about the advantages and disadvantages of wearing an insulin pump.
Then, you start to learn how to operate the pump and to become comfortable with this treatment.
It may take several months to get comfortable with the pump, but if you will be highly motivated, able to operate the pump, and willing to test blood glucose frequently, than you will adjust to it shortly.
What are the advantages of using the insulin pump?
- Insulin pumps deliver insulin more accurately than injections.
- There are fewer fluctuations in blood glucose levels.
- Greater flexibility of meals, exercise, and daily schedule.
- It causes lower HbA1c.
- It can improve your quality of life and can make diabetes treatment and management much easier.
So, what's the catch?
- Well, it's more expensive.
- It is a constant reminder of your diabetes.
- It may require a full day at the hospital or clinic to be trained.
- There is a risk of Diabetic Ketoacidosis if one of the components is malfunctioning, such as the pump battery if it's discharged, or if the insulin reservoir runs empty.
But the increasing use of insulin pumps throughout the world shows that most pump wearers agree the advantages outweigh the disadvantages.
Read more here about insulin pumps.
|
Returm from Diabetes Treatment to Diabetes Guide |